Prognostic Modeling and Decision Matrices: Evaluating a Bump on Gum After Root Canal
In the management of compromised dentition, the recurrence of pathology presents a pivotal decision point. The presentation of a bump on gum after root canal—indicative of chronic apical abscess—moves the tooth from a "stable" category to a "failing" category. As a senior consultant at Luxe Smile Studio, my role is to evaluate the strategic viability of retaining such a tooth. We must weigh the prognosis of retreatment against the predictability of extraction and implant replacement. This is not merely about treating an infection; it is about forecasting the 5- and 10-year survival capability of the dental unit in the context of the patient's overall health and financial investment.
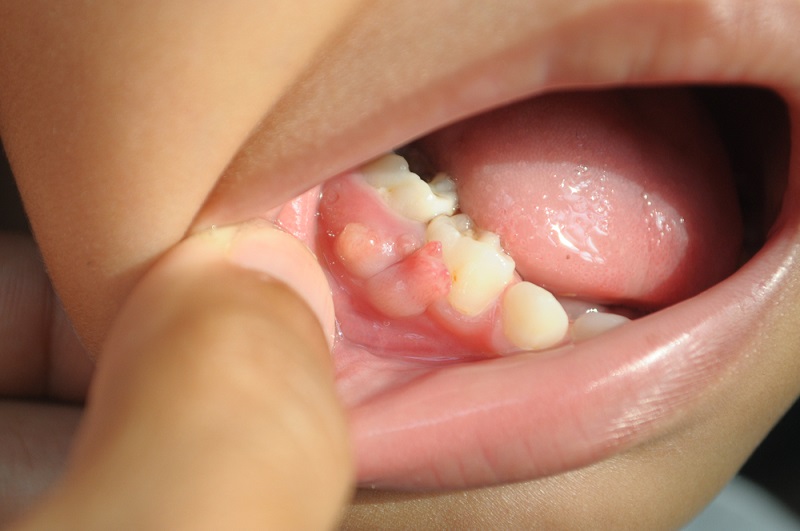
The Retreatment Viability Matrix
Not all failing root canals are candidates for a second attempt.
Assessing Restorability and Access
When a patient presents with a bump on gum after root canal, we must assess the obstacles to retreatment. Is there a long post cemented in the canal? Is the canal curvature severe? Is there calcification?
- Favorable Prognosis: If the failure is due to a missed canal or leaking crown, and the root structure is robust, non-surgical retreatment has a high success rate (80-85%).
- Guarded Prognosis: If the previous treatment looks technically perfect on X-ray, the failure implies a resistant extra-radicular infection (biofilm on the outside of the root). In this case, surgical intervention (apicoectomy) offers a better prognosis than simple retreatment.
The Bone Loss Factor
The sinus tract indicates active bone destruction.
Critical Bone Volume
The bump on gum after root canal is essentially a drain for a bony cavity. We must evaluate the size of this lesion via CBCT (3D imaging). If the lesion has eroded the buccal cortical plate significantly, or encroaches on the sinus or nerve canal, the risk of retaining the tooth increases. Prolonged retention of a failing tooth consumes the very bone needed for a future implant. Strategically, it is sometimes wiser to extract a tooth with a bump on gum after root canal sooner rather than later to preserve the alveolar ridge for replacement therapy.
Risk Factors for Surgical Intervention
Apicoectomy (cutting the root tip) is often the last line of defense.
Crown-to-Root Ratio
Microsurgery removes the infected root tip (3mm) and seals the end. However, this shortens the root. If the tooth already has short roots or significant periodontal bone loss, removing another 3mm may destabilize the tooth. A bump on gum after root canal on a tooth with a poor crown-to-root ratio is often a terminal sign. The strategic advice here is often extraction, as the surgical solution would only yield a transient extension of life (2-3 years) before mechanical failure occurs.
Patient-Centered Decision Making
The clinical data must be overlaid with the patient’s values.
The Cost of Heroics
Retaining a tooth with a bump on gum after root canal often involves expensive disassembly (removing crowns/posts), retreatment, and new restoration. The cost can exceed that of an implant. If the prognosis is guarded (<70% success chance), I advise patients to consider the "cost of heroics." Are they willing to invest time and money into a tooth that may still fail? For strategic teeth (like a bridge abutment), the risk may be worth it. For a single tooth with no strategic value, replacement is often the more predictable long-term pathway.
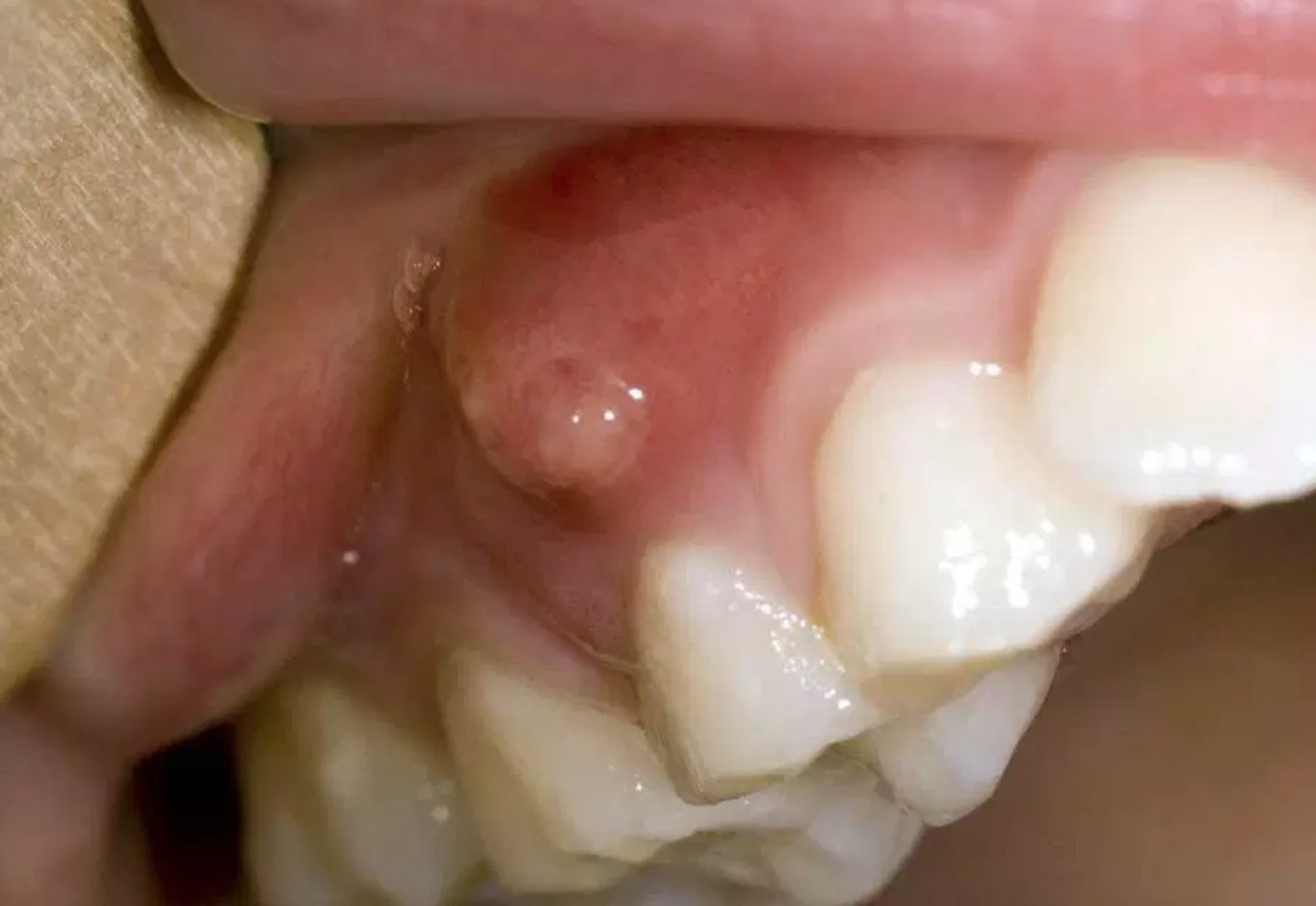
A boil on gum after root canal is a definitive sign of failure, but not necessarily a sign of loss. By applying rigorous prognostic criteria—evaluating bone volume, root structure, and infection type—we can guide the patient toward the solution (retention or extraction) that offers the highest probability of long-term health and stability.




