Photon Attenuation and Sensor Geometry: Engineering Perspectives on Are Dental X-Rays Safe
The technical review division at Luxe Smile Studio investigates the biomechanical and structural engineering parameters governing modern dental equipment. Analyzing the query regarding whether are dental X-rays safe demands a departure from biological abstraction, requiring instead a rigorous mechanical audit of the physical hardware utilized in contemporary clinics. The safe administration of electromagnetic energy is a function of precise electron deceleration, beam collimation engineering, and the quantum efficiency of solid-state image receptors. This documentation provides a technical breakdown of the hardware modifications and physics principles that systematically restrict patient exposure to negligible thresholds.
Bremsstrahlung Radiation Production and Are Dental X-Rays Safe
The genesis of the imaging process occurs within the evacuated glass envelope of the X-ray tube head. The engineering challenge is generating a high-energy photon beam with strict dimensional and energetic boundaries. The system utilizes a cathode filament, typically constructed of tungsten, which undergoes thermionic emission when an electrical current is applied. The resulting electron cloud is accelerated across a high-voltage potential difference toward a focal spot on a tungsten anode target.
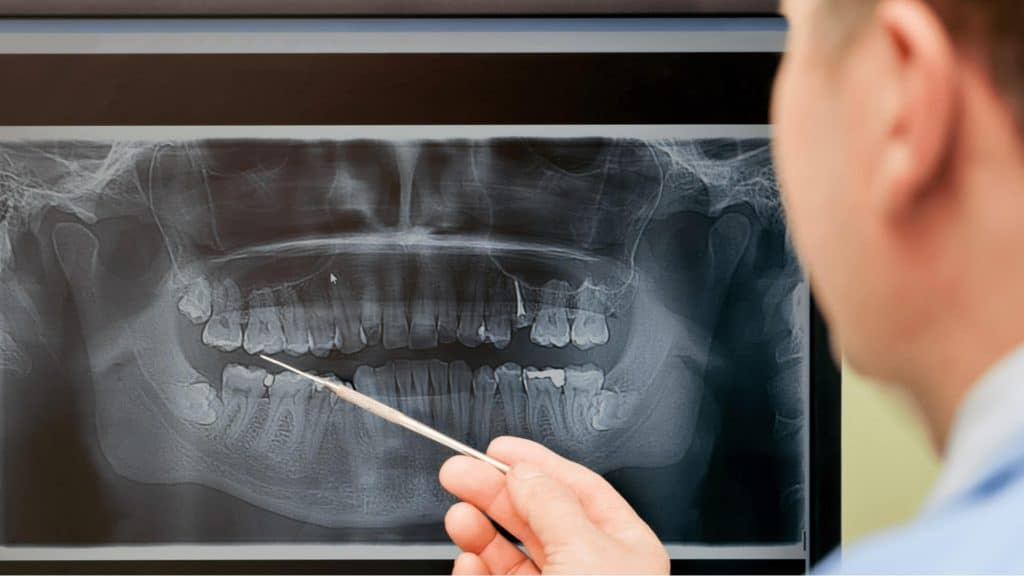
Upon impact, the kinetic energy of the electrons is converted via Bremsstrahlung (braking radiation) interactions. The technical basis for determining whether are dental X-rays safe lies in the filtration of this resulting polyenergetic beam. The beam inherently contains low-energy, long-wavelength photons that lack the penetrative force to exit the patient's soft tissue and reach the sensor. These "soft" photons contribute solely to patient dose without adding diagnostic value. To engineer a safer exposure profile, inherent and added aluminum filtration barriers (typically equivalent to 1.5 to 2.5 mm of aluminum) are structurally integrated into the tube head aperture. These filters physically absorb the non-diagnostic low-energy spectrum, ensuring that only the high-energy, highly penetrative "hard" photons interact with the patient, thereby optimizing the signal-to-noise ratio and dramatically reducing the absorbed tissue dose.
Collimator Engineering Ensuring Are Dental X-Rays Safe
Once the filtered beam exits the tube housing, its geometric divergence must be strictly controlled to prevent the irradiation of peripheral, non-target anatomy. The mechanical component responsible for this spatial restriction is the collimator, a dense metallic cylinder or rectangle, typically constructed of lead.
The engineering shift from traditional circular collimation to rectangular collimation represents a massive advancement in patient safety. A circular collimator produces a beam diameter of approximately 2.75 inches at the patient's skin, exposing a surface area significantly larger than the standard image receptor. In contrast, a modern rectangular collimator is engineered to restrict the photon beam to the exact dimensional footprint of a size 2 digital sensor. This geometric constraint reduces the total volume of irradiated facial tissue by an impressive fifty to sixty percent. Furthermore, restricting the primary beam reduces the generation of Compton scatter radiation within the patient's tissues, which not only lowers the systemic dose but also prevents scatter-induced image fogging, enhancing the overall diagnostic contrast.
CMOS Sensor Quantum Efficiency and Dose Reduction
The final technical variable dictating the safety of the procedure is the physical capture of the attenuated photons. The transition from photochemical silver halide film to solid-state digital radiography relies on the implementation of Complementary Metal-Oxide-Semiconductor (CMOS) or Charge-Coupled Device (CCD) active pixel sensors.
These digital receptors are constructed with a scintillating layer, frequently utilizing cesium iodide, which efficiently converts incident X-ray photons into visible light photons. This light is subsequently directed through fiber-optic faceplates into the silicon pixel array, where it is converted into a measurable electrical charge. The core engineering advantage of CMOS technology is its extraordinarily high Detective Quantum Efficiency (DQE). Because the sensor is exponentially more sensitive to photon interactions than traditional analog film, the X-ray generator needs to be activated for only a fraction of a second—often as brief as 0.05 seconds per exposure. By drastically shortening the temporal duration of the primary beam emission, the total kinetic energy delivered to the patient is minimized, establishing a robust, technically engineered foundation for the safety of digital intraoral imaging.
When patients inevitably ask, "are dental X-rays safe?", the scientific consensus is clear: the operational safety of dental radiography is not accidental; it is a meticulously engineered outcome. Through the implementation of aluminum beam filtration, rectangular collimation geometry, and high-efficiency solid-state CMOS receptors, the hardware systematically mitigates unnecessary exposure. The integration of these technical controls ensures that diagnostic imaging functions within the strictest parameters of biophysical safety.



